
Integrative Health (IH) faculty are piloting the “Whole Health” model at the UW Health Arboretum Clinic.
“This model focuses on what matters most to people, which increases the chances of their actively participating in the health care process,” explains Adam Rindfleisch, MPhil, MD, DFMCH associate professor and medical director of the UW Health IH program.
To help patients understand their health in a way that goes beyond traditional disease management and wellness, Integrative Health (IH) faculty from the UW Department of Family Medicine and Community Health (DFMCH) are piloting the “Whole Health” model at the UW Health Arboretum Clinic.
The model is offered to patients who come to the clinic for longer primary-care office visits, such as physical exams. Patients who opt to participate first complete a personal health inventory, which encourages them to consider aspects of their health that are most important to them.
Specifically, patients rate their current state—and where they would like to be in the future—in eight areas:
- Working the Body (energy and flexibility)
- Recharge (sleep and refresh)
- Food and Drink (nourish and fuel)
- Personal Development (personal life and work life)
- Family, Friends and Coworkers (relationships)
- Spirit and Soul (growing and connecting)
- Surroundings (physical and emotional)
- Power of the Mind (relaxing and healing)
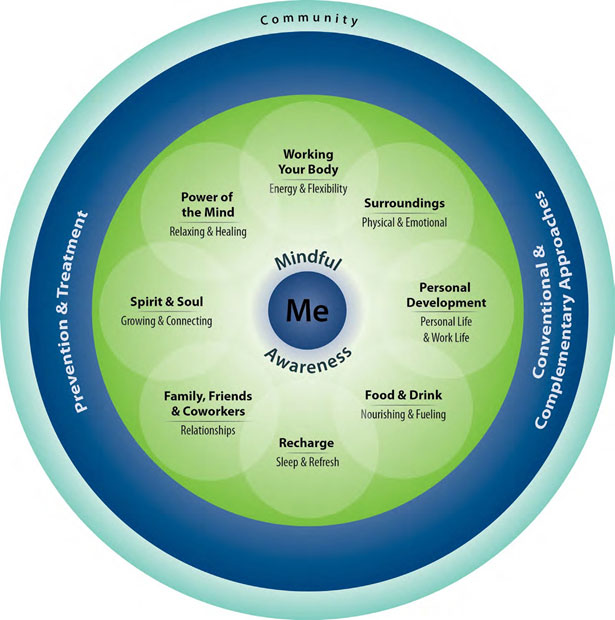
The Circle of Health graphic illustrates how patients can think about the Whole Health model. The inner dark blue circle represents an individual’s values and aspirations. The green circle represents self-care and everyday choices. The outer dark blue circle represents professional medical care (traditional and complementary). The outer light blue circle represents community support. (Circle of Health courtesy of the VHA Office of Patient Centered Care & Cultural Transformation.)
Patients also rate their overall physical and mental well-being and their sense of their day-to-day life.
The inventory is designed to help patients better understand what really matters to them, why they want to be healthy and what their best possible life might look like.
Patients then work with their physician to determine how self-care, professional care (including traditional and complementary approaches) and their community can best support them.
Focusing on What Matters Most
“This model focuses on what matters most to people, which increases the chances of their actively participating in the health care process,” explains Adam Rindfleisch, MPhil, MD, DFMCH associate professor and medical director of the UW Health IH program.
“It empowers them around what they can do to optimize their health,” he continues. “It also offers them a chance to build a team that can help, including by providing guidance around complementary approaches and community resources.”
So far, patients have responded positively to the “Whole Health” model. Some are curious about the different approach, which provides an opportunity for clinicians to discuss the importance of overall well-being.
“Blood glucose and blood pressure control are important, but we don’t want to lose sight of the reasons they are important,” explains Greta Kuphal, MD, who practices at the Arboretum Clinic and offers the model to her patients.
“We want to support someone in improving their overall health, so they can reach a goal they set for themselves—whether it be climbing a mountain, walking a daughter down the aisle or being a ‘spry old woman’. This is the journey we walk with patients.”
Advancing Health and Well-Being
The “Whole Health” model is informed by a national collaboration between the DFMCH and the Veteran’s Health Administration’s Office of Patient Centered Care & Cultural Transformation.
That collaboration aims to advance an approach to health care in which clinicians and patients partner to co-create health and well-being.
The “Whole Health” pilot began at the Arboretum clinic in January 2016. If it continues to be successful there, it may be rolled out to other UW Health primary care clinics.
The IH program, in collaboration with UW Health Wellness, is also holding a two-day conference in May to introduce the “Whole Health” model more broadly to UW Health clinicians and leaders.
To learn more about the model, contact Dr. Rindflesich.
Published: April 2017
